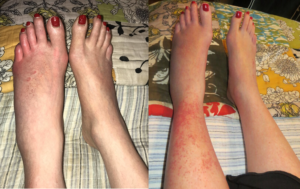
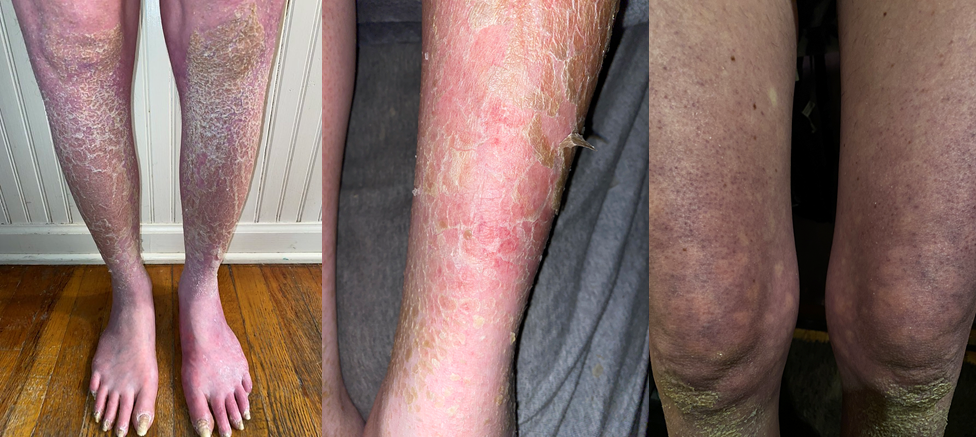
A Concussion, an Infection and the Slow Spiral of Declining Health
Our daughter started ballet at 2.5 years old, and by 5 years old she had started competitions and had decided she was going to become a professional ballerina. She was talented, had an amazing work ethic and completely loved her life of ballet, friends and school. She was a very happy child, bright and bubbly and she woke up everyday super excited about what was going to be happening that day. From a very early age, our daughter showed determination, stubbornness and a quiet, but strong competitiveness.
In October 2016, when she was 12 years old, she got a severe concussion, and her whole life stopped for nearly 3 months. She stayed in her bedroom in the dark, couldn’t read, slept for most of the day and even trying to tie her shoelaces gave her an intense headache. After months of no improvement, we took her to a chiropractor, who told us her neck was out and she wouldn’t have gotten better until it was put back in properly. Our daughter floated out of that appointment so happy that she nearly felt back to her normal self. The chiropractor gave us an information sheet about Thiamine/B1 Vitamin at the time, but we didn’t really take any notice apart from trying to give her some more marmite (yeast spread) as it suggested.
Then in September 2017, both our daughter and our older son suddenly became very ill with vomiting, diarrhoea, rashes, headaches, stomach pain, joint pain, and bright red palms. Our older son had more intense symptoms, and also had extreme nose bleeds and petechial rashes – he was admitted to hospital where they found his liver and spleen were enlarged but they couldn’t work out what was wrong. Our son had recently come back from a school trip to Vietnam – we were trying to find if there was a link to Vietnam but he had already been home for a couple of weeks so the hospital didn’t test for any illnesses from Vietnam. After weeks of this illness, we were told our daughter had Mono/Epstein Barr Virus and that this was causing her illness and it was completely unrelated with our son’s illness. We found this extremely odd that they could have mostly the same symptoms at exactly the same time, but as our son was more acute and in hospital, we were just concentrating on trying to get both of them well.
Since then, our daughter has never fully recovered. She started not sleeping, and constantly having body pains and headaches. She was sent to a paediatrician who diagnosed her with Child Migraines and told us she would outgrow them and was given melatonin for sleep. The melatonin worked for 3 nights and then completely stopped working. Our daughter started to put on weight, and would look puffy in the face, and she lost her menstrual period even though she was gaining weight. She was always tired, always had body pains and slowly but surely lost her sparkle.
Declining Metabolic Function and Weight Gain
At the end of 2017 when she was 13 years old, she lost her place in the national ballet training program. Our daughter was extremely stoic at this point, and was determined to get a professional career without the training academy’s help. Throughout 2018 she continued to put on weight, no matter how healthy she ate or what she ate, and still didn’t have a menstrual period. We saw doctors and nutritionists, but they couldn’t explain why her weight continued to increase or they would tell us there was nothing wrong. Our daughter became quiet, withdrawn, easily irritated and frustrated and stopped being interested in anything or anyone. She continued to work at her ballet, and the only time she would ‘light up’ would be on stage, as she was still trying to compete. During 2018, she gained 10kg/22lbs while being on a very strict nutrition plan. She auditioned for a ballet academy to start at the beginning of 2019 and was accepted; she was happy but in a tired way, and she knew that she would need to stop gaining weight but had no idea how she was going to do that when she had already been trying so hard.
In February 2019 we saw a naturopath who diagnosed our daughter with Adrenal Fatigue, and said her thyroid needed support, and that she still had lingering Epstein Barr Virus in her system. The naturopath pointed to our daughter always wanting salt as an indicator of adrenal fatigue. She was put on some herbal remedies for her immune system, inflammation and liver, adrenal and thyroid support, and relaxation/sleep support as well as Epstein Barr Virus liquid drops to help her immune system recognise the lingering EB virus in her system.
The weight started to instantly melt off, her sleeping improved and we felt we finally had some answers and a solution. Our daughter was happy with the weight loss, but still struggled with her other symptoms: dizziness, dry/gritty eyes, chest pain, tiredness, muscle and joint pains, extremely sore lower and upper back pain, brain fog, very low blood pressure, daily headaches, daily sore throat, complete lack of energy and occasionally sore under her right ribs (later on she told us that she couldn’t sweat, no matter how hard or long she exercised).
A month after starting the herbal remedies, she had her first panic attack during rehearsal for a school production – she had no idea what was happening and it took a long time to calm her down. Her mental and emotional state continued to decline, it was a daily struggle to do anything; she always had to push through every single day. We continued to take our daughter to the doctors for the sore throats, tiredness, headaches etc. but we were always told there was nothing wrong with her. During this time she got an infected toenail, and ended up being on antibiotics for twice as long as usual as it wouldn’t heal. The naturopath added in additional supplements to help, and eventually her toe got better.
Even though she was still losing weight, our daughter became very apathetic and would stay in her room – we would try to talk to her every day, try to reach her but she was shut off emotionally. Then we ran out of one of the herbal supplements, and suddenly she began to gain weight again – she gained 2.8kg/6.2lbs in 2 weeks. Once we got her back on the herbal supplement she began to lose weight again, but it seemed to be slower and less effective. Our daughter got to 51.3kg (she is 5ft7 inches tall) and she was happy, and her ballet teachers told her to not lose any further weight as she was fine at the weight she was.
Hair Loss, Pale Skin, and Skyrocketing Weight
Halfway during 2019, our daughter’s hair started to fall out in clumps, it got to the point where she was too scared to wash or comb it, as it was falling out so much. We noticed our daughter was extremely pale, and at times she looked translucent. The naturopath put her on iron pills and told us to massage her scalp, but it didn’t really make a difference. The naturopath didn’t think she needed to be on the adrenal/thyroid support any longer, and was changing her supplements. Our daughter’s weight then skyrocketed, and our relationship with the naturopath started to deteriorate as she kept implying that we were starving our daughter and we felt she wasn’t able to answer our questions on why one particular supplement seemed to be the only one that would help our daughter lose weight, but she still had the other symptoms that were getting worse.
We took our daughter to other GP doctors, trying to explain her symptoms and asking for her thyroid to be checked, but we were continuously brushed off and they would look at our daughter and say it was just normal teenage hormonal stuff and there was nothing wrong. In our gut we felt there was something drastically wrong, but nobody would listen to us. We started to hate going to the doctors, going through her symptoms only to be told again and again there was nothing wrong with her, and being looked at like we had the problem, not our daughter. We started trying to research things ourselves, started tracking and monitoring everything she ate/did/sleep patterns. The naturopath would change the supplements and our daughters weight would skyrocket – we would then put her back on the original supplements and again she would start to lose weight, but every time it was less effective.
Low Metabolic Rate, Low Estradiol, Yeast and Bacterial Overgrowth, Constipation and Parasites
At the beginning of 2020, our daughter’s weight was going back up significantly and it seemed that the original supplement was no longer working at all. We realised that our daughter’s face and neck seemed to be more swollen on the left side, but couldn’t find any reason why it would be like this. Our daughter started to get new symptoms around this time as well – from not being able to sweat at all, she started to have extreme sweating everywhere, and started to get hot flushes and night sweating. We noticed that the hair on her upper lip was more noticeable/darker, and she started to get a small patch of hair just under the middle of her lower lip as well. She also started to get a very bloated around her stomach area, and couldn’t pull it in no matter how hard she tried.
In February 2020, we decided to try and get testing done ourselves, and found a functional doctor who supplied a variety of tests. We got a hormone and thyroid test, as well as a MTHFR gene mutation test. We thought if we could show our doctor some factual data, we might be taken more seriously. The functional doctor advised us to also do an Organic Acid urine test, which we did as well. The test results came back saying that our daughter’s total estrogen was so low that it was at the level of a post-menopausal woman, but the functional doctor thought that was because she was a dancer. The organic acid test picked up that she was in a hypometabolic state; again with the reason given that this was because she was an athlete. The organic acid test also showed that she had a significantly high amount of yeast and bacterial overgrowth in her gut, which would cause inflammation system wide and insulin resistance.
The functional doctor wanted to test for parasites as well, so we did a complete microbiome mapping test using a stool sample. While taking the stool sample, we were surprised that our daughter could only produce tiny, rock-hard little pebbles and we questioned her about it, we then found that she was constipated but she thought passing tiny pebble-type stools only every 3-5 days was normal.
While we were waiting for the microbiome mapping results, the functional doctor prescribed a total of 30 supplements/remedies as well as adrenal support liquid drops – these were to cover supporting biochemical pathways, weight management, cognitive support, anti-inflammatories, detoxification, liver support, hormonal metabolism, adrenal and energy support, amino acids to support cellular energy, mitochondrial NRG multivitamins to support cellular health, l-tryptophan to support sleep and neurotransmitter mood support. During this time she was also advised to stop all dairy (she was already gluten/sugar free and very low carb). We did take all of these tests results to our GP doctor, but were advised that they didn’t recognise these tests.
After a week of the new supplements, we noticed a complete shift in our daughter’s energy level and emotional/mental state. We were relieved to have our daughter’s personality back – it was literally like a heavy, suffocating blanket had been taken off her and she could finally think, feel and breathe again – it was a huge difference seeing her not having to mentally struggle through every single day. We did a lot of talking with her and she finally admitted just how numb she had felt to everything, but also scared that this was how she was going to be for the rest of her life. The supplements did nothing for her weight, which continued to increase, and some of the other physical symptoms, but we were now clinging to the information that we knew she could lose the weight, and that now she could also be better emotionally and mentally with higher energy levels – we just had to figure out what was stopping her from having all of these things at the same time.
In May 2020, the microbiome mapping results came back, and we were surprised to find that our daughter an extreme level of a parasite in her system, called Blastocystis hominis, as well as an overgrowth of Rhodotorula fungi and a couple of other opportunistic bacterial overgrowths. The functional doctor immediately put her on a parasite/bacterial/yeast eradication protocol that was to be for two months, and then we were supposed to follow that with 6 months of a rejuvenation program.
When our daughter found out it was a parasite that was making her sick, she was absolutely ecstatic. She had loved ballet her whole life, but thought it was ballet making her sick so had been pushing it away which had been hurting her emotionally – it hurt her to think that the thing she loved the most was hurting her. Now that she knew it was instead a parasite making her sick, she felt she could allow herself to love ballet again. While waiting for the herbal remedies for the eradication protocol, we started to research the parasite, and started to become very concerned at just how difficult it was to get rid of it, and the devastating symptoms/damage that it could do.
Looking at other protocols that were used to get rid of this particular parasite, the remedies weren’t the same as the ones prescribed by our functional doctor, so we questioned if these particular remedies had been used for this parasite before and if they were successful. We were assured that these remedies had been used and were definitely successful.
Failed Treatments and Inconclusive Diagnoses
Our daughter started on Australian Oil of Oregano, 6 capsules a day totalling 900mg of essential oil each day, as well as 6 capsules of a GI-Microbe remedy for worms. After a week she noticed she had a very itchy bottom and a sore stomach. Our GP doctor wanted to check for PCOS because of the lack of menstrual period and her hair falling out, so our daughter had a pelvic ultrasound 6 days after starting the Oil of Oregano. The sonographer couldn’t see anything in the ultrasound because of the amount of gas (it looked like billowing black clouds on the screen), so after a lot of discussion due to our daughter’s age, she had an internal ultrasound. The sonographer was surprised that it was still hard to see anything due to the amount of gas, so could only see one ovary and a small piece of her uterus, which the sonographer said looked good and didn’t indicate there was PCOS.
During the following week our daughter’s stomach pain became more intense, and her weight was skyrocketing. We started to get very concerned at her escalating reactions but kept being reassured by the functional doctor that this was normal. After 20 days of being on the Oil of Oregano we decided to take our daughter off all of the supplements as we felt they were just making her worse. All of the literature on the parasite Blastocystis advises that you need to wait 8 weeks before doing PCR stool testing to see if the parasite has been eradicated or not. We are currently waiting until 10 August 2020 at the earliest to be able to test to see if the parasite is gone. Since this Oregano treatment, her stools are now every day and better consistency (they were floating which we think is fat malabsorption issues?) and her menstrual period has returned. Her appetite has also reduced, and she isn’t craving carbs and sugar as she has now revealed she used to.
Since then our daughter’s weight has continued to increase at a rapid rate – in total from 27 January 2020 to 31 July 20202 she has gained 14.5kg/32lbs, with 10kg/22lbs being in the last 2.5 months. She can physically no longer do ballet, so she sits and watches in class instead. After joining a Facebook group for the parasite Blastocystis, we have been seeing a naturopath in Australia via Zoom who had the parasite themselves. We are currently waiting on a SIBO breath test results as the naturopath thinks our daughter also has SIBO. We spend all of our time trying to research all of our daughter’s symptoms, while watching her physically deteriorate. It has totally consumed our family.
Where We Are Now: Was It Thiamine All Along?
Our daughter is in a better mental/emotional space, but doesn’t physically recognise her body at all. Even our daughter’s orthodontist asked why she was so swollen in her face, especially the left side – but the doctors still don’t think there is anything wrong. Our daughter’s physiotherapist is too scared to touch her, as she is so swollen. We spend every day crying at some point. While researching SIBO symptoms, we came across a comment about Thiamine deficiency, so started to research and bought the book “Thiamine Deficiency Disease, Dysautonomia, and High Calorie Malnutrition”. Reading about the swelling of the face, and that it is fluid retention in the body was a revelation. But because of what happened with the Oil of Oregano, we are too scared to try doing something on our own and potentially making it worse, and the more we research, more of the other co-factors, we keep finding and things to be careful of. We have been to our GP doctor asking them to investigate if it could be beriberi, so they have started doing blood tests, but then we found in the appointment notes that the doctor still thinks our daughter looks well, so we are disappointed that it looks like they are not taking this potential diagnosis seriously.
Currently we’re waiting on Allithiamine and Lipothiamine to arrive from Australia, as we can’t purchase it here in New Zealand, but with Covid-19 there are huge delays in postage. We have started our daughter on 150mg of Benfotiamine (even that was extremely difficult to find in New Zealand) but at this stage we are hesitant to just ramp up the dosage to see instant results. We took our daughter back to the chiropractor who now advises that her kidneys/bladder aren’t working properly, and also that her vagus nerve isn’t working either. Just this week, we have taken her to an acupuncturist to try and help with the fluid retention, and they’re concerned about her heart and liver and just how swollen she is. We have added in legumes to her diet to help with bile function/detoxification and her stools are now increasing and no longer floating. We are now wondering if maybe she was hypoglycaemic as well.
Reading the comments on the Thiamine Deficiency Facebook group, we should also be looking at potassium supplementation, but conversely you shouldn’t supplement with potassium if there is something wrong with your kidneys. With the doctors not believing us, alternative practitioners wanting to potentially only push their own agenda/supplements or not fully understanding the full consequences of their remedies, or not being able to find out what the root cause of the problem is, and the conflicting information all over the internet, we are completely lost/scared/petrified/confused and feel a huge pressure to fix our daughter and it feels like time is rapidly running out. The stress on us as parents is completely overwhelming, and financially we feel like we are throwing money at this ever-increasing problem and the money is fast running out. We feel that every day is getting worse than the day before, and our hope has faded to a tiny pinprick of light. Gathering all of the information together for the doctors/alternative practitioners/supplements/nutritionist plans/tests looks absolutely ludicrous, but when you’re in the thick of it you’re completely desperate to find anything that could potentially fix your child. Then when it doesn’t work, or it makes the symptoms worse, the guilt is huge.
We’re hoping that by publishing her story on Hormones Matter, others might look at our daughter’s case history, and confirm what is wrong, explain it to us so that it makes sense, and help us fix her in a safe way.
Current Diet and Supplements
Below is a snapshot of our daughter’s typical diet and supplement regime. Please note, the Benfotiamine was begun only recently.
| Breakfast | Morning Tea | Lunch | Afternoon Tea | Dinner | Water/Teas and Remedies before bed |
| Douglas Labs Ultrazyme x 1 | 1 large gold kiwifruit | Douglas Labs Ultrazyme x 1 | 50gm Coconut Yoghurt | 105gm Roast Beef | 3 x Magnesium Citrate (Pure Encapsulations) |
| 2 Egg Muffins – Bacon/Veg | 2 teaspoon sunflower seeds | 90gm tin pink salmon | with probiotics | 0.5 cup roast pumpkin | |
| 2 Tablespoons Pumpkin Seeds | 1 cup Almond Milk | 1 cup green Kale/Pak Choi (homegrown) | 10 almonds | 0.5 cup broccoli | |
| 1 Tablespoon Apple Cider Vinegar | 2 x Tran-Q | 1 cup tomatoes | 1 Apple | 0.5 cup peas | |
| 2 Brazil Nuts | 0.5 cup cucumber | 2 x Tran-Q | |||
| 1 scoop Orthoplex Gut Rx | 0.5 cup grated carrot | ||||
| 1 X HPA Essentials Tablet | 0.25 cup brown rice | ||||
| ** 1 x Doctors Best Benfotiamine 150 | 1 Tablespoon mashed Avocado | ||||
| 1 teaspoon flaxseed oil | |||||
| 1 tablespoon lemon juice | |||||
| 1 X HPA Essentials | |||||
| 1 scoop Orthoplex Gut Rx |
** Benfotiamine was just recently added as of July 25, 2020.
We Need Your Help
More people than ever are reading Hormones Matter, a testament to the need for independent voices in health and medicine. We are not funded and accept limited advertising. Unlike many health sites, we don’t force you to purchase a subscription. We believe health information should be open to all. If you read Hormones Matter, like it, please help support it. Contribute now.
Yes, I would like to support Hormones Matter.
Image by Dimitris Doukas from Pixabay.
This story was published originally on August 10, 2020.