Hormones Matter is a health oriented website edited by Chandler Marrs, PhD. She has long recognized the need for people to report their “mystery illnesses”, simply because they are slipping through the cracks in modern medicine. My association with Dr. Marrs is a very fruitful one because we both have the same viewpoint. This viewpoint embraces the concept that the present disease model is antiquated and badly needs to be revised. In a recent post, I have defined what we mean by a “medical model”. We both have found that a common health problem, largely unrecognized for its true cause, is a polysymptomatic illness that is almost invariably labeled psychosomatic. I will try to explain.
Food, Energy, and Illness
Much of our food is broken down to glucose, the primary fuel of the brain. This has given rise to a common concept that taking virtually any form of sugar is a way to develop “quick energy”. Before the processing of sugar in the body was understood, athletes would sometimes load up on it. We now know that this defeats the purpose. Very much like a car where an excess of gasoline “chokes” the engine, an excess of sugar has a very similar effect, particularly in the brain. An additional effect of sugar is the extremely sweet taste that sends a signal from the tongue to centers in the brain that gives the person an extreme sense of pleasure. It has been shown in animal studies that sugar is more addictive than cocaine and a book was published in 1973 entitled “Sweet and Dangerous”. The author, Dr. John Yudkin, was a professor of nutritional studies in a major London hospital. He was able to show that sugar was the cause of many modern diseases. It is indeed hard for people to understand that such an appreciated delight is dangerous to our health. If we turn to nature, you will find that sugar is never found in its free state. It is always found in fruit and vegetables where fiber is a vital component in its processing. The sweet taste from eating a banana or an orange is the way that Mother Nature designed it and it is a healthy way of experiencing a sweet taste.
Glucose is burned (oxidized) in cellular “engines” (mitochondria) and it is a very complex process. The net result is energy that is stored in a chemical substance known as adenosine triphosphate (ATP). The nearest analogy would be a battery because the energy that drives all our mental and physical functions is electrical in nature.
By far and away the commonest personal story posted on Hormones Matter is a polysymptomatic illness that is the result of inefficient energy transduction and its major effect is in the brain. To put it as simply as possible, food is not being converted into energy in sufficient amount to meet the stresses of merely being alive. The most susceptible part of the brain that is affected is the part that controls our ability to adapt to living in an environment that is essentially hostile. Using a specialized nervous system and a bunch of glands that produce hormones, this part of the brain signals every organ in the body to participate. Now obviously, if no energy were produced we would die and that is indeed a major cause of death. However this common polysymptomatic illness affecting so many people is based on an inefficient energy production, not a complete lack. It can vary in its degree of severity depending on nutritional and genetic factors. The dominant effect is “psychological”, symptoms such as undue fatigue, depression, anxiety and anger. It can run the gamut of our emotional reactions. In fact, because of its emotional implications, I have suggested that the common state of violence in America is a reflection of our uncontrolled hedonism. Can a person nursing a perceived grievance become violent if the emotional controls are too easily activated?
Energy lack is quickly recognized as dangerous by the brain. It causes a sense of panic to be felt by the affected person. That is why “panic attacks” have been recognized incorrectly as a “psychological disease that requires a medicine to tranquilize the patient” whereas they really represent a fight-or-flight reflex, naturally designed to get the affected person “out of perceived danger, i.e. energy deficiency”. The affected person seeks medical help, but this effect in the brain is seen by most physicians as “psychological”, as though the patient is inventing the symptoms. The diagnosis is, “it’s all in your head”. The irony is that although the symptoms are indeed the result of a function “in the head”, they are evidence of a sick brain lacking in adequate energy and therefore have an understandable origin and meaning. Also, the symptoms are easily erased by administration of non-caloric nutrient supplements when they are initially experienced. If allowed to continue unchecked, sometimes for years, they may lead to the irreversible damage characterized as a neurodegenerative disease.
Because the dominant effect is in the part of the brain that controls the specialized nervous system, it begins to send out exaggerated “panic” signals to the organs of the body. The result is a variable assortment of physical effects— heart palpitations, breathing problems, diarrhea, often alternating with constipation, whole body pain, migraine headaches, nasal congestion, nausea with or without vomiting, chest or abdominal pain, pins and needles etc. In other words, any organ in the body may be activated or non-activated because the pattern of our adaptive mind/body machinery is adversely affected. The very important point is this: each and every action of the brain/body union requires energy, even sleep!
Perhaps the most common symptom is severe fatigue and this has given rise to a common diagnosis of Chronic Fatigue Syndrome (CFS). It is worth noting that it is often associated with Irritable Bowel Syndrome (IBS) and it seems to be medically accepted that two diseases, both of “unknown cause” can occur in a patient at the same time. That seems to be a product of illogical thinking based on the present medical model.
Share Your Story
Anyone encountering this website is encouraged to write his or her health story and share it as a blog post. These stories help raise awareness about the scope of illnesses affecting us all and add to the knowledge base. To share your health story, send us a note here.
If you have specific questions about health and illness, we recommend that you “surf” the site because there are many posts on a variety of topics with long and detailed comment threads, one or more of which may be similar to your own story and may answer your questions.
We Need Your Help
More people than ever are reading Hormones Matter, a testament to the need for independent voices in health and medicine. We are not funded and accept limited advertising. Unlike many health sites, we don’t force you to purchase a subscription. We believe health information should be open to all. If you read Hormones Matter, like it, please help support it. Contribute now.
Yes, I would like to support Hormones Matter.
Image by Leandro De Carvalho from Pixabay .
This article was published originally on December 2, 2019.
Rest in peace Derrick Lonsdale, May 2024.








































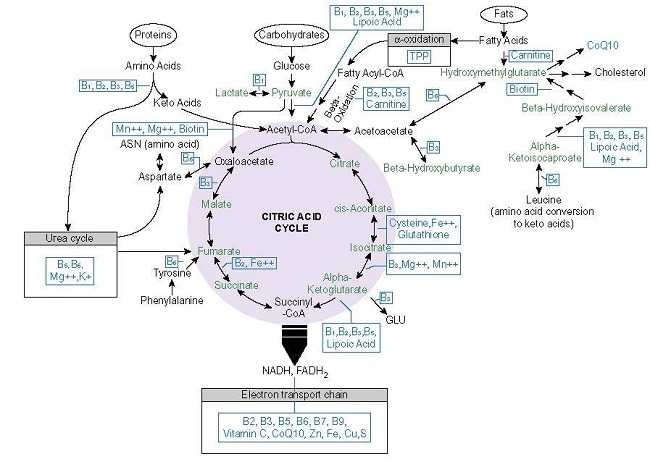 A few things should be pointed out. First, while these nutrients are required by everyone for proper mitochondrial functioning, not everyone needs to supplement with each one, or even sometimes any of them, although that is becoming increasingly rare with modern dietary patterns. Secondly, notice how many times and where vitamin B1 (thiamine) appears in this chart. It is at the entry points of the entire system and at various junctures throughout. This suggests that among all of the nutrients required for healthy mitochondria, thiamine is particularly important. Unfortunately, it is the one nutrient that is so often ignored or missed in testing. Indeed, that is why we wrote the book. Thirdly, notice how many vitamins are required to process the food we eat into ATP. Contrary to popular opinion, we need more than simply empty calories. For the foods we eat to be converted into ATP, there are multitude of vitamins and minerals required that may or may not be included in sufficient density with the macronutrients we consume daily. Finally, not discussed in this chart, but discussed in great detail in the book, synthetic chemicals, whether in form of pharmaceuticals, industrial, environmental, or food production, damage the mitochondria. Some deplete nutrients directly, while others damage aspects of mitochondrial functioning that necessitate increased nutrient density for the enzyme machinery to work. Of course, underlying all of this, are the genetic variables that each of us brings to the table. These influence how well or poorly we metabolize any of these nutrients from the get-go. All of this combines to make nutrient therapies complicated.
A few things should be pointed out. First, while these nutrients are required by everyone for proper mitochondrial functioning, not everyone needs to supplement with each one, or even sometimes any of them, although that is becoming increasingly rare with modern dietary patterns. Secondly, notice how many times and where vitamin B1 (thiamine) appears in this chart. It is at the entry points of the entire system and at various junctures throughout. This suggests that among all of the nutrients required for healthy mitochondria, thiamine is particularly important. Unfortunately, it is the one nutrient that is so often ignored or missed in testing. Indeed, that is why we wrote the book. Thirdly, notice how many vitamins are required to process the food we eat into ATP. Contrary to popular opinion, we need more than simply empty calories. For the foods we eat to be converted into ATP, there are multitude of vitamins and minerals required that may or may not be included in sufficient density with the macronutrients we consume daily. Finally, not discussed in this chart, but discussed in great detail in the book, synthetic chemicals, whether in form of pharmaceuticals, industrial, environmental, or food production, damage the mitochondria. Some deplete nutrients directly, while others damage aspects of mitochondrial functioning that necessitate increased nutrient density for the enzyme machinery to work. Of course, underlying all of this, are the genetic variables that each of us brings to the table. These influence how well or poorly we metabolize any of these nutrients from the get-go. All of this combines to make nutrient therapies complicated.

